Mobile Surgical Lights: A Comprehensive Guide to Portable Operating Room Illumination
Imagine this: a multi-vehicle collision on a remote highway. The nearest Level I trauma center is an hour away by air. In a makeshift medical tent, a team works frantically to stabilize a critical patient, but the sun has set, and the portable generators are straining. The surgeon needs to perform an emergency thoracotomy—a life-saving procedure to access the chest—but the available light is diffuse, casting deep shadows that obscure vital anatomy. In this moment, the difference between life and death can literally come down to lumens. This is the uncompromising reality where mobile surgical lights transition from a piece of equipment to a lifeline.
In the controlled environment of a main operating room (OR), illumination is so meticulously engineered we often take it for granted. Yet, proper surgical lighting is non-negotiable. It is the foundation upon which visual acuity, surgical precision, and ultimately, patient safety are built. Mobile surgical lights embody the critical fusion of this non-negotiable need with essential flexibility. They bring the gold standard of OR illumination to any location, whether filling a gap in a traditional suite or creating an OR where none existed.
This guide serves as an authoritative resource for surgeons, anesthesiologists, nursing staff, hospital procurement teams, and facility managers. We will dissect the technology, unequivocal benefits, rigorous selection criteria, and vital best practices for mobile surgical lighting. The insights herein are compiled from industry standards (such as those from the Illuminating Engineering Society), clinical studies on surgical performance, and expert perspectives from clinical engineering, ensuring the information is not only accurate but practically applicable.
What Are Mobile Surgical Lights? Defining Portable OR Illumination
At their core, mobile surgical lights are self-contained, high-intensity illumination systems mounted on a maneuverable floor stand. They are engineered to deliver light quality that meets or exceeds the stringent requirements of surgical procedures, but with the inherent advantage of portability.
Core Definition and Key Components
A typical mobile surgical light consists of several key components:
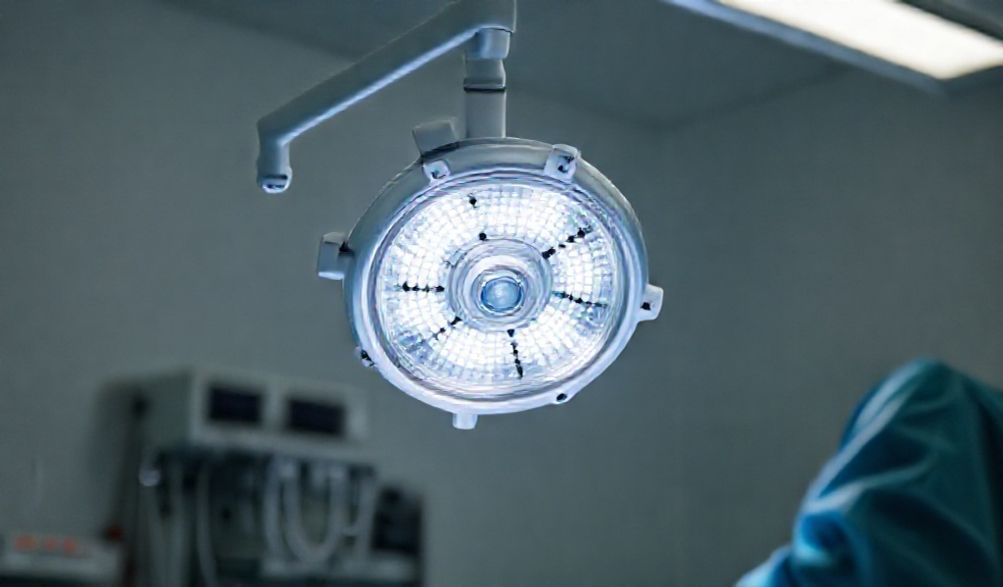
* The Light Head: This is the business end, housing an array of high-output LEDs (Light Emitting Diodes). Modern designs focus on creating homogeneous, shadow-reduced light fields. The head often allows for adjustment of intensity (measured in lux) and color temperature.
* The Articulating Boom: This arm connects the light head to the column. It features multiple points of articulation (knuckles or joints) that allow the light to be positioned precisely—extended out, pulled back, raised, lowered, and rotated—to achieve the optimal angle over the surgical site.
* The Mobile Base and Column: A sturdy, often weighted, base on lockable casters provides stability to prevent tipping. The column raises and lowers the entire boom assembly. The base houses control electronics and, crucially, a rechargeable battery system for backup power.
* Control System: This can include handles on the light head for manual positioning, touch panels or dials on the column for adjusting light settings, and sometimes remote controls or touchless gesture controls for maintaining a sterile field.
The fundamental differentiation from fixed, ceiling-mounted systems is independence. A fixed light is a part of the room’s architecture. A mobile light is a piece of clinical equipment that can be moved to the need.
Primary Use Cases and Clinical Applications
The versatility of mobile surgical lights makes them indispensable across a wide spectrum of care:
* Emergency and Trauma Surgeries: In crowded ER bays or trauma rooms where a patient cannot be moved to an OR, a mobile light can be rushed in to provide immediate, procedural-grade lighting.
* Field Hospitals, Military Medicine, and Disaster Response: As the opening scenario illustrates, these lights are foundational for deployable surgical units, providing critical care in austere environments without reliable infrastructure.
* Supplemental Lighting in Main ORs: During complex procedures like spinal or multi-organ transplants, a primary ceiling light may be supplemented with a mobile unit to illuminate a deep cavity from a second angle, effectively eliminating shadows.
* Outpatient Surgery Centers and Clinics: For facilities that perform a variety of procedures but lack the budget or infrastructure for multiple fixed installations per room, a few mobile lights can be shared and positioned as needed, maximizing flexibility and cost-efficiency.
* Veterinary Surgical Suites: High-quality illumination is equally vital in advanced veterinary medicine, and mobile lights offer the same benefits of adaptability for different animal sizes and procedure types.
Critical Advantages of Implementing Mobile Surgical Lighting
The decision to integrate mobile surgical lights is driven by more than just convenience; it’s an investment in clinical capability, safety, and operational intelligence.
Unmatched Flexibility and OR Layout Freedom
Fixed lights dictate surgical approach to some degree. Mobile lights liberate the surgical team. The light can be positioned to follow the procedure, not the other way around. Whether it’s an unconventional patient position, a need to approach from a specific angle, or an OR with physical obstructions, a mobile light can be maneuvered to deliver optimal illumination precisely where it’s needed, dramatically reducing frustrating and dangerous shadows cast by the surgeon’s own hands and instruments.
Enhanced Patient Safety and Surgical Outcomes
This is the paramount advantage. Superior lighting is directly correlated with superior outcomes. A study published in Surgical Endoscopy and other journals has highlighted how improved illumination reduces visual fatigue and eye strain among surgeons, which is a known factor in human error. High lux levels and excellent color rendering (achieved through adjustable color temperature, typically 4000K-5500K) allow for exceptional differentiation between tissue types, vasculature, and subtle color changes—critical for identifying margins, controlling bleeding, and preserving vital structures. By enabling greater precision, mobile lights that meet these high standards directly contribute to reduced complication rates and improved patient recovery.
Cost-Effectiveness and Operational Efficiency
From a financial perspective, mobile lights present a compelling case:
* Lower Initial Capital Outlay: Installing a single high-end fixed ceiling light can cost significantly more than a premium mobile unit, not including the architectural and electrical work required.
* Maximized Asset Utilization: One mobile light can serve multiple procedure rooms. In an ambulatory surgery center, a light can be used in an orthopedic case in the morning and a plastic surgery case in the afternoon, simply by rolling it to the next room.
* Rapid Deployment for Emergencies: There is no faster way to upgrade the lighting capability of a non-OR space than wheeling in a mobile light. This readiness can save crucial minutes in a code or trauma situation.
Key Technical Specifications to Evaluate Before Purchase
Selecting a mobile surgical light requires a forensic look at its technical specifications. These are not mere numbers; they are promises of clinical performance.
Illumination Quality: Lux, Color Temperature, and Shadow Management
- Lux (Illuminance): This measures the intensity of light falling on the surgical field. General surgery may require 40,000 to 160,000 lux at the center of the field. Deep cavity or microsurgery demands the higher end of this range. Always verify the lux at a specified working distance (e.g., 1 meter).
- Color Temperature (CCT): Measured in Kelvins (K), this determines how “warm” (yellow/red) or “cool” (blue/white) the light appears. Adjustable CCT (e.g., from 3500K to 5000K) is a key feature. Cooler temperatures enhance contrast and are often preferred for general surgery, while warmer tones can be easier on the eyes during long procedures and may improve visualization of vascular structures.
- Shadow Management: This is achieved through multi-point source design. Instead of one bright bulb, the light head contains multiple LED clusters arranged in a ring or pattern. When a surgeon’s hand obstructs one cluster, the others fill in the shadow, dramatically reducing its depth and obscurity. Look for terms like “deep cavity illumination” and “shadow dilution.”
Mobility and Stability: Design and Maneuverability
A light that is hard to move or prone to drifting is worse than useless—it’s a hazard.
* Base and Casters: The base must be low-profile to avoid tripping but weighted for stability. Large, easy-rolling casters with positive locking mechanisms (often a central foot pedal) are essential.
* Boom Articulation: The boom should have a sufficient reach (often >150cm) and multiple, fluidly moving joints. It should stay securely in position once set, with no “creep” or sagging over time. Counterbalanced systems allow for smooth, effortless positioning.
Sterility and Cleanliness: Infection Control Design
The unit must withstand the rigorous decontamination protocols of a surgical environment.
* Materials and Surfaces: All exteriors should be seamless, non-porous, and resistant to common hospital disinfectants. Absence of crevices, seams, and textured surfaces where bio-burden can accumulate is critical.
* Sealed Optics: The light head should be completely sealed to prevent fluid ingress and dust accumulation on the internal optics or LEDs. Anti-reflective coatings on external lenses should also be durable and easy to clean.
How to Choose the Right Mobile Surgical Light: A Step-by-Step Guide
Navigating the market requires a structured approach. Follow these steps to make an informed, evidence-based decision.
Step 1: Assess Your Clinical Needs and Facility Workflow
Begin with an internal audit. Ask:
* What types of procedures will the light support? (General, orthopedic, plastic, neurosurgery?)
* What are the room sizes and layouts? Are there space constraints?
* How frequently will it be used? (Daily workhorse or emergency backup?)
* Who will be positioning it? (Surgeons, nurses, techs?)
Step 2: Compare Top Brands and Models (Vendor-Neutral Overview)
Create a comparison matrix. Evaluate models based on the specs discussed: central lux, CCT range, boom reach, battery life, weight, and warranty. Reputable manufacturers will have a long history in medical lighting. Focus on the specifications that match your needs assessment, rather than brand name alone.
Step 3: Prioritize Safety Certifications and Compliance
This is non-negotiable. Any device used in surgery must carry relevant medical device certifications. Mandatory marks include:
* FDA Clearance (or equivalent in your region).
* ISO 13485: Quality Management System for medical devices.
* IEC 60601-1: The international standard for safety and essential performance of medical electrical equipment.
Step 4: Consider Total Cost of Ownership (TCO)
Look beyond the sticker price:
* Initial Cost: The purchase price of the unit.
* Lifespan & Maintenance: LEDs rated for 50,000-100,000 hours may last 10+ years. What is the cost and process for eventual replacement?
* Service Contracts: Availability and cost of preventative maintenance and repair services.
* Battery Replacement: Plan for the periodic replacement of the backup battery system.
Best Practices for Operation, Maintenance, and Safety
Owning the equipment is only half the battle; proper use and care ensure it performs reliably for years.
Daily Operational Protocols for Clinical Staff
- Positioning: Move the unit with the boom folded and lowered. Position the base so the column is behind the surgeon, allowing the boom to extend over their shoulder without obstruction. Ensure all casters are locked before the procedure begins.
- Pre-Surgical Check: Before draping, turn on the light and adjust the intensity and focus to the surgeon’s preference. Verify the battery is charged.
Scheduled Maintenance and Cleaning Procedures
- Cleaning: After every use, following facility protocol, wipe down all surfaces with a hospital-grade disinfectant. Pay special attention to handles and control panels. Never spray liquid directly onto the light head; apply to a cloth first.
- Maintenance: Adhere strictly to the manufacturer’s scheduled service intervals. This typically includes inspection of mechanical joints, electrical safety checks, and verification of light output metrics by clinical engineering.
Troubleshooting Common Issues
- Flickering or Dim Light: Check the power connection first. If on battery, plug in the unit. Persistent issues may indicate a failing LED driver or power supply.
- Stiff or Drifting Boom: This may require lubrication or adjustment of the tensioning mechanism by a qualified technician.
- Unresponsive Controls: Perform a power cycle. If problems persist,
CRITICAL WARNING: Mobile surgical lights are complex medical devices. Do not attempt internal repairs. Any malfunction must be reported immediately to your facility’s Biomedical Engineering department or the equipment manufacturer’s service team.
Frequently Asked Questions (FAQ) About Mobile Surgical Lights
Q1: Can a mobile surgical light provide the same light quality as a fixed ceiling light?
A: Yes, absolutely. Modern high-end mobile surgical lights are engineered to meet the same stringent optical standards (lux, color rendering, shadow reduction) as fixed lights. For the vast majority of procedures, they are clinically equivalent. The primary advantage of fixed lights is permanent, unobstructed overhead positioning, which may still be preferred in ultra-specialized, high-volume suites.
Q2: How long does the battery last on a mobile surgical light, and what happens if it fails during surgery?
A: Most units offer 2 to 4 hours of full-intensity battery backup. Standard protocol is to keep the light plugged into mains power during surgery, with the battery acting as an uninterruptible power supply (UPS). In the event of a total power failure, the battery seamlessly takes over. Facilities should have a backup plan, such as a secondary mobile light or battery-powered headlamps, for extremely prolonged outages.
Q3: Are mobile surgical lights difficult to sterilize and keep clean for infection control?
A: No, when designed and used correctly. The key is selecting a model with a smooth, sealed, and crevice-free exterior. As with all OR equipment, strict adherence to the manufacturer’s cleaning instructions using approved disinfectants is mandatory to maintain infection control standards.
Q4: What is the typical lifespan of the LEDs in a mobile surgical light?
A: Medical-grade LED arrays are remarkably durable, with typical rated lifespans between 50,000 and 100,000 hours. Under normal surgical schedules (e.g., 10 hours a day, 250 days a year), this translates to 15-20 years of use before light output degrades to a point requiring replacement.
Q5: Do mobile lights require special electrical outlets or room preparation?
A: Generally, no special preparation is needed. They operate on standard hospital-grade electrical outlets (e.g., 110-120V or 220-240V). The primary room requirement is sufficient clear floor space around the surgical table to position the unit stably without creating a tripping hazard or obstructing the movement of staff and equipment.
Conclusion
Mobile surgical lights represent a paradigm shift in surgical illumination, transforming light from a fixed architectural feature into a dynamic clinical tool. They empower healthcare providers to deliver high-standard surgical care with unprecedented flexibility, whether in a state-of-the-art hospital, a busy outpatient clinic, or a disaster relief zone. The benefits—enhanced surgical precision, improved patient safety, and operational cost-efficiency—are clear and compelling.
Choosing the right mobile surgical light is a significant clinical and financial decision that demands careful consideration. Use this guide as your foundational framework for evaluation. Scrutinize specifications against your clinical needs, prioritize safety certifications, and always factor in the total cost of ownership.
The information presented here is rooted in industry expertise and a commitment to supporting the medical community. To make the best decision for your facility, we strongly recommend taking the next critical step: Contact reputable medical equipment suppliers to request detailed specifications and, most importantly, arrange a hands-on clinical trial or demonstration. Seeing the light quality and maneuverability in a simulated environment is the ultimate test, ensuring your investment will shine brightly for years to come, illuminating the path to better patient outcomes.
p>