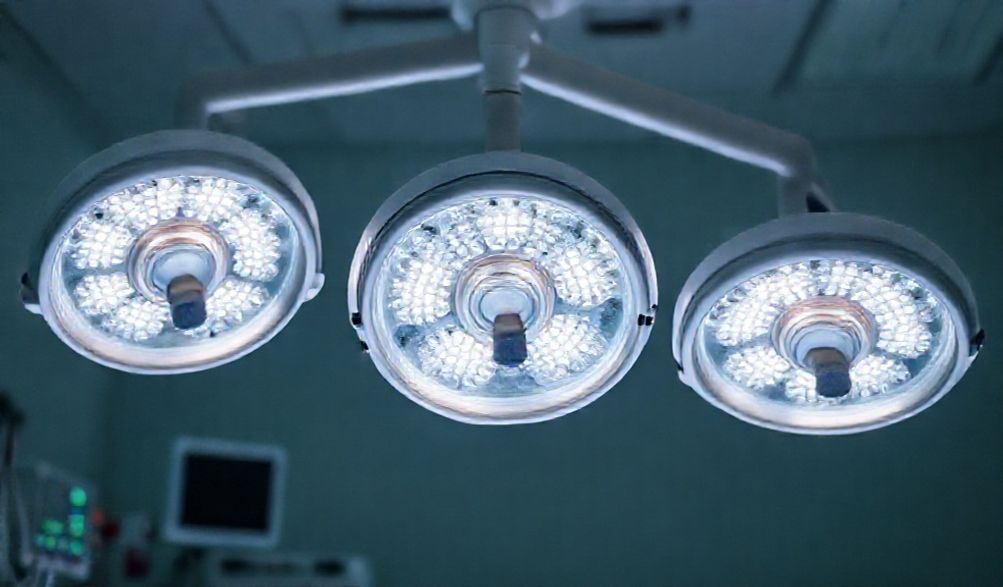
The Ultimate Guide to LED Surgical Lights: Benefits, Technology & Selection Criteria
Introduction
In the high-stakes environment of an operating room, every detail matters. The surgeon’s skill, the sterility of the instruments, and the precision of the technology all converge to determine a patient’s outcome. But what if one of the most fundamental tools—the very quality of light illuminating the surgical field—could directly impact patient safety and surgical precision? For decades, this critical component was a given, but today, a technological revolution is redefining illumination in surgery.
This comprehensive guide is designed to be your definitive, evidence-based resource on LED surgical lights. Whether you are a surgeon, an operating room manager, a clinical engineer, or part of a hospital procurement team, the decision to upgrade or invest in new surgical lighting is significant. Synthesizing insights from clinical studies, manufacturer white papers, and established industry standards, we will cut through the technical jargon to provide clear, actionable information.
We understand you are likely researching to make an informed purchase, justify an upgrade to administration, or simply understand the tangible clinical advantages of modern systems. This post promises a clear breakdown of the core technology, the proven benefits, the essential selection criteria, and a glimpse into the future of surgical illumination. By the end, you will be equipped with the knowledge to evaluate LED surgical lights not just as a piece of equipment, but as a vital contributor to surgical success.
What Are LED Surgical Lights? Understanding the Core Technology
At their essence, LED surgical lights are illumination systems that use Light Emitting Diodes (LEDs) as their light source, specifically engineered to meet the rigorous demands of the operating room. But to appreciate their value, it’s important to understand the journey that led to their dominance.
From Halogen to LED: The Evolution of Surgical Illumination
The history of surgical lighting is a story of chasing the perfect beam. For much of the 20th century, incandescent and later halogen lights were the standard. Halogen lights, an improvement on their predecessors, offered brighter, whiter light than typical incandescent bulbs. They were followed by xenon lights, which provided intense, daylight-like illumination and became a benchmark for color quality.
However, these technologies came with inherent drawbacks. Halogen and xenon bulbs are incredibly inefficient, converting most of their energy into heat rather than light. This “hot light” posed risks of tissue drying (desiccation) and increased ambient temperature in the OR. Their lifespans were short—often just 1,000 to 2,000 hours—leading to frequent, costly bulb replacements and surgical downtime. Furthermore, their light output would decay over time, gradually dimming without the surgical team necessarily noticing.
The paradigm shift began with the advent of solid-state LED technology. Originally used in electronics and consumer lighting, LEDs were adapted for surgical use, offering a solution to nearly every limitation of traditional lighting. This transition represents one of the most significant advancements in OR infrastructure in recent decades.
How LED Surgical Lights Work: Key Components Explained
An LED surgical light is more than just a cluster of bulbs. It’s a sophisticated system of integrated components:
- LED Arrays and Chipsets: Instead of a single large bulb, hundreds of tiny, high-intensity LED chips are arranged in a dense array. This multi-source design is fundamental to reducing shadows; if an instrument blocks some LEDs, others fill in the gaps from different angles. The quality of the semiconductor material (often using blue LEDs with a phosphor coating to create white light) determines the light’s purity and efficiency.
- Heat Dissipation Systems: While LEDs are far more efficient, they still generate heat at the semiconductor junction. Effective thermal management is critical to maintaining LED lifespan and performance. This is achieved through advanced heat sinks (often aluminum fins) that passively draw heat away, and sometimes active cooling with internal fans. Crucially, this heat is managed at the source and not projected forward as infrared radiation onto the surgical site, creating the “cold light” effect.
- Optical Lenses and Light Field Homogenization: A complex system of secondary optics, including reflectors and lenses, sits over the LED array. These components collimate and blend the light from each individual chip to create a perfectly homogeneous field. This eliminates multiple shadows and “hot spots,” providing even, consistent illumination across the entire defined diameter, from center to edge.
- Color Rendering Index (CRI) and Correlated Color Temperature (CCT): These are the metrics of light quality.
- L'IRC measures a light source’s ability to reveal the true colors of objects compared to natural daylight (which has a CRI of 100). In surgery, a CRI >95 is essential for accurately differentiating between tissues, arteries, veins, and organs, and for identifying subtle variations in color that indicate oxygenation or pathology.
- CCT, measured in Kelvins (K), describes the hue of the white light. “Warm” light is around 3500K (yellowish), while “cool” light is 5000K+ (bluish). Many LED surgical lights offer adjustable CCT (e.g., from 4000K to 5000K), allowing surgeons to tailor the light to the procedure—cooler for enhanced contrast in deep cavities, warmer for surface tissue work.
Top 5 Clinical & Operational Benefits of Modern LED Surgical Lights
The shift to LED is not merely a change of bulb; it’s an upgrade that delivers profound benefits across clinical, operational, and financial domains.
1. Enhanced Visual Accuracy & Reduced Surgeon Fatigue
The primary goal of any surgical light is to enable the surgeon to see clearly. LED systems excel through advanced shadow control via their multi-source design and homogenizing optics. This is particularly vital in deep-cavity surgeries (like thoracic or pelvic procedures), where traditional lights struggle. Furthermore, the ability to adjust color temperature can reduce eye strain. A light that mimics natural daylight (high CRI, tunable CCT) helps maintain the surgeon’s visual acuity and color perception over long procedures, reducing cognitive load and fatigue, which are known factors in human error.
2. Improved Patient Safety and Surgical Outcomes
Patient safety is directly enhanced in two key ways. First, the “cold light” characteristic of LEDs—minimal infrared emission—significantly reduces the risk of thermal injury and tissue desiccation at the surgical site. This promotes better healing and lowers a potential vector for infection. Second, unlike halogen bulbs that dim over time, LEDs maintain a consistent luminosity throughout their entire lifespan. Surgeons are always working with the intended, optimal light level, removing a variable that could subtly impact precision and decision-making.
3. Significant Long-Term Cost Savings and Sustainability
While the initial capital outlay for an LED system can be higher, the Ne vous fiez pas uniquement au prix d'achat. Calculez le is dramatically lower. Consider: an LED light engine boasts a lifespan of 50 000 heures ou plus. Compared to a halogen bulb at 1,500 hours, this translates to over a decade of operation without a bulb change, eliminating procurement, inventory, and labor costs for replacements. Operationally, LEDs are 60-70% more energy-efficient, slashing electricity costs. From a sustainability perspective, LEDs contain no mercury, generate less waste due to their longevity, and reduce the hospital’s carbon footprint through lower energy consumption.
4. Unmatched Reliability and Reduced Operational Downtime
The solid-state nature of LEDs makes them highly resistant to shock and vibration. There is no fragile filament to break. This inherent robustness, combined with the extraordinary lifespan, means surgical lights are far less likely to fail during a critical procedure. The nightmare scenario of a bulb burning out mid-surgery is virtually eliminated. This reliability ensures the OR schedule flows smoothly, maximizing room utilization and surgical throughput.
5. Design Flexibility and Integration Readiness
Modern LED surgical lights are designed with the modern OR in mind. They are typically lighter and more compact than their predecessors, allowing for greater maneuverability and reach from ceiling mounts. Their digital control systems are primed for integration with other OR technologies, such as surgical booms, video recording systems, and room control panels. This future-proofs the investment as operating rooms evolve towards greater connectivity and data integration.
How to Choose the Right LED Surgical Light: A Procurement Checklist
Selecting the right system requires moving beyond brand names and focusing on specifications that align with your clinical needs and infrastructure.
Assessing Technical Specifications: Lumens, Lux, and Depth of Illumination
- Lux & Illuminance: This is the key metric for brightness at the surgical field. General surgery typically requires 40,000 to 160,000 lux at a defined distance (e.g., 1 meter). Specialized procedures like neurosurgery or microsurgery may demand even higher levels. Ensure the quoted lux is measured at the center et un the edge of the light field.
- Light Field Diameter & Depth of Illumination: The system should offer a tunable light field (e.g., from a focused 10cm spot to a wide 30cm field). More importantly, evaluate its depth-of-illumination—the ability to maintain a consistent lux level even as the light head is moved farther from the target. A good system will maintain homogeneity and intensity over a range of 60-100cm.
- CRI and CCT: Do not compromise on color quality. Insist on a CRI of 95 or higher and, ideally, a system with adjustable CCT to provide flexibility for different surgical specialties.
Evaluating Ergonomic Design & Ease of Use
- Sterility & Cleanability: The light head must have a completely boîtier scellé et lisse with no crevices where contaminants can lodge. It should withstand frequent cleaning with hospital-grade disinfectants without degrading.
- Maniabilité : Test the range of motion. Can it be easily positioned over any part of the patient without the surgeon contorting? Is the handle intuitive and placed for sterile access? Consider the balance—does it stay in position without drift?
- Control Panel: Controls should be intuitive, responsive, and accessible. Look for features like programmable memory settings for different procedure types, touchscreen interfaces, and potentially sterile remote controls.
Compatibility and Integration with Your Operating Room
- Options de fixation : Decide between plafonnière (fixed, track, or single-point) systems for permanent ORs and mobile floor stands for multi-purpose rooms or minor procedure areas.
- Integration Capability: If you have or plan for a hybrid OR, endoscopic suites, or video recording, ensure the light system has data ports and communication protocols (like CAN bus) to integrate with surgical booms, cameras, and room control systems.
- Infrastructure Compliance: Verify the electrical requirements and ensure your facility’s ceiling structure can support the weight and movement of the chosen system. Engage your clinical engineering or facilities team early in the process.
The Future of Surgical Lighting: Smart Integration and AI
The evolution of LED surgical lights is moving towards intelligent, context-aware systems that are fully integrated into the digital OR ecosystem.
Adaptive Lighting and Automated Settings
Imagine a light that automatically adjusts its intensity and color temperature based on the image displayed on the primary surgical monitor, optimizing the surgeon’s view of both the field and the screen. Future systems may use ambient light sensors or input from the surgical video feed to make these adjustments in real-time. Pre-set “procedure profiles” (e.g., “Cardiac,” “Laparoscopic,” “Orthopedic”) could be activated automatically based on the OR schedule, setting the perfect light environment before the team even enters the room.
Integration with Hybrid ORs and Image-Guided Surgery
In advanced environments like hybrid ORs, where real-time imaging (CT, MRI, fluoroscopy) guides the procedure, lighting must complement, not interfere. Future lights will synchronize with imaging modalities, perhaps dimming automatically during a scan and instantly returning to preset levels afterward. They could also be programmed to provide specific illumination patterns that align with surgical navigation systems, enhancing the fusion of visual and digital data for the surgeon.
Frequently Asked Questions (FAQ) About LED Surgical Lights
Q1: What is the typical lifespan of an LED surgical light, and how does it compare to halogen?
R : LED surgical lights have a typical rated lifespan of 50 000 heures ou plus. In contrast, halogen bulbs last between 1,000 and 2,000 hours. This means one LED system can outlast 25-50 halogen bulb replacements. It’s important to note that “lifespan” for LEDs usually refers to the point (L70) where light output depreciates to 70% of its original value, not a complete failure.
Q2: Are LED surgical lights really “cold” lights? Do they produce any heat?
R : They are called “cold lights” because they emit minimal infrared (IR) radiation directly onto the surgical site, unlike halogen bulbs which project significant IR heat. However, LEDs do generate heat at the semiconductor chip itself. This heat is effectively drawn away from the light-emitting surface via advanced heat sinks and thermal management systems located within the light head, protecting both the electronics and the patient.
Q : Quelle est l'importance de l'Indice de Rendu des Couleurs (IRC) pour la chirurgie ?
R : It is critically important. A high CRI (>90, and preferably >95) is essential for accurate tissue differentiation. It allows surgeons to clearly distinguish between arterial and venous blood, identify subtle variations in tissue health, and recognize anatomical landmarks based on color. A low CRI can mask these nuances, potentially impacting surgical judgment and outcomes.
Q4 : Les systèmes d'éclairage chirurgical existants peuvent-ils être modernisés avec la technologie LED ?
R : Parfois. Certains fabricants proposent des kits ou modules de modernisation LED pour leurs anciens modèles. Le principal avantage est un coût initial inférieur. Cependant, les inconvénients potentiels incluent : le nouveau module LED peut ne pas être parfaitement optimisé pour l'optique du boîtier d'origine, réduisant ainsi les performances ; l'ergonomie et les commandes restent obsolètes ; et le système mécanique vieillissant peut être proche de la fin de sa durée de vie utile. Un remplacement complet du système est souvent le meilleur investissement à long terme. Consultez toujours un ingénieur biomédical ou le fabricant.
Q5 : Quels sont les principaux protocoles de stérilisation et de maintenance pour les lumières LED ?
R : Suivez toujours les instructions d'utilisation spécifiques du fabricant (IFU). Les protocoles généraux incluent : n'utiliser que des désinfectants approuvés, non abrasifs et non corrosifs sur les surfaces scellées ; éviter les pulvérisations à haute pression sur les articulations et les commandes ; et s'assurer que la lumière est éteinte et refroidie avant le nettoyage. La maintenance doit inclure une inspection régulière par l'ingénierie clinique pour l'intégrité mécanique, la vérification du flux lumineux (niveaux de lux) et l'étalonnage des capteurs et des commandes selon les recommandations.
Conclusion
La transition vers l'éclairage chirurgical LED représente bien plus qu'une simple mise à niveau technologique. Il s'agit d'une amélioration fondamentale de l'environnement chirurgical qui touche tous les aspects des soins : améliorer la vision du chirurgien, protéger le patient, rationaliser les opérations et réduire les coûts à long terme. Les preuves sont claires — les avantages d'un contrôle supérieur des ombres, d'une émission de lumière froide, d'une fidélité chromatique exceptionnelle et d'une remarquable durabilité font des systèmes LED la norme incontestée pour la salle d'opération moderne.
Investir dans un éclairage chirurgical LED de haute qualité, c'est investir dans votre infrastructure clinique de base. C'est une décision qui privilégie les performances fondées sur des preuves et la valeur totale sur la durée de vie, plutôt que le prix initial. Pour la suite, nous vous encourageons à utiliser les critères présentés ici comme cadre d'évaluation.
Vos prochaines étapes : Consultez un fournisseur certifié d'équipements biomédicaux qui comprend les flux de travail cliniques. Demandez une démonstration en direct, voire un essai dans un environnement de bloc opératoire simulé, pour constater les différences par vous-même. Donnez à votre équipe d'achat une liste de contrôle détaillée des spécifications pour garantir que vous comparez les systèmes sur un pied d'égalité.
Alors que la chirurgie poursuit sa trajectoire vers les techniques mini-invasives, la robotique et l'intégration des données, l'éclairage avancé cessera d'être perçu comme un simple outil. Il sera reconnu comme une composante fondamentale et intelligente des soins aux patients — un partenaire silencieux de la précision, œuvrant à garantir que chaque intervention soit réalisée sous la meilleure lumière possible.
p>